When $60 Becomes $800: How to Catch (and Fix) Health Insurance Errors
A real-life lesson in why you must audit your Explanation of Benefits.
We often assume that when the pharmacist rings up a total, or when a medical bill arrives in the mail, the number is correct. We assume the insurance computer “knows” our plan.
But we also know that the insurance computer (and even the claims processors) have a history of applying the plan incorrectly (or inconsistently).
In January I had accepted that the “computer” knew our new plan for our prescriptions —and it nearly cost my family over $1,300 in a single month.

From Advocate to Patient
For years, I essentially worked two jobs. By day, I was a Speech-Language Pathologist working full-time. By night, I often spent three hours at a time, multiple nights a week, on the phone with insurance companies fighting for my own coverage. I learned early on that whether you are an educator advocating for a student, provider advocating for a patient, or a patient advocating for yourself, the system will often default to “No” unless you prove otherwise.
Now, living with chronic illness and on long-term disability, I no longer have that kind of energy to spare. My “work” today is largely just managing my own health. So when a computer glitch recently caused our pharmacy bills to skyrocket, it wasn’t just a financial error—it was a drain on the limited energy I have to survive.
I’m sharing this story not just as a professional who knows the paperwork, but as a patient who knows the exhaustion. I want to help you catch these errors quickly so you don’t have to spend your evenings fighting for the coverage you’ve already paid for.
The “Glitch”: When the Math Doesn’t Math
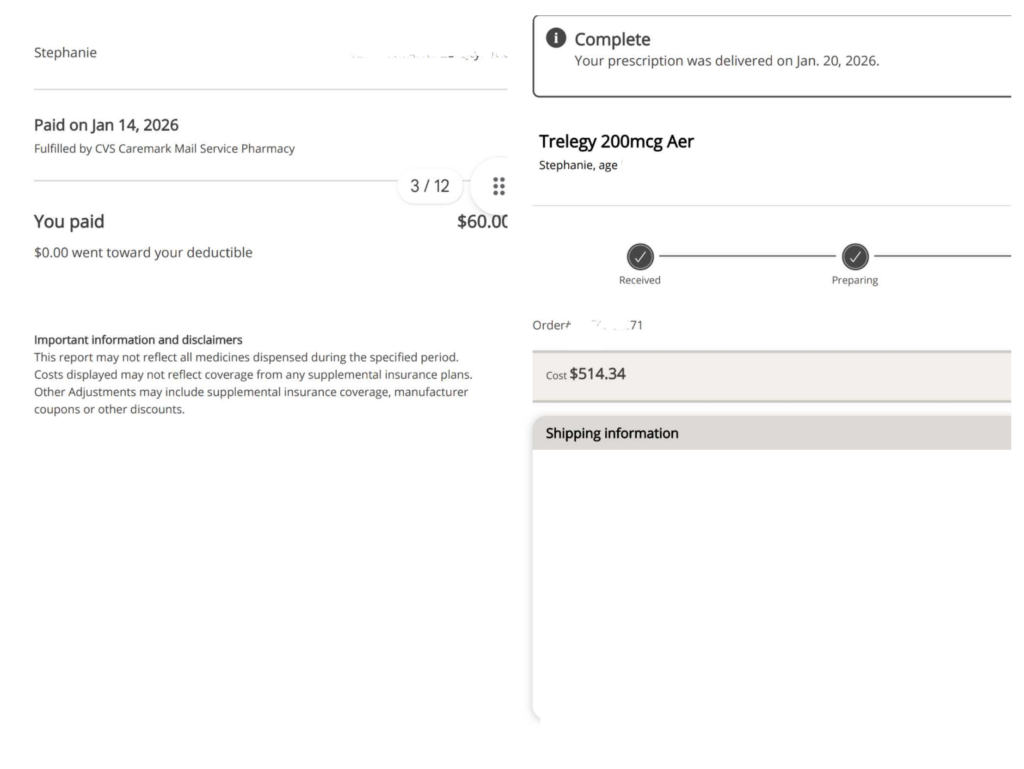
The “Glitch”: When the Math Doesn’t Math The situation started simply enough: My husband went to pick up a routine prescription. Instead of his usual $60 copay, he was charged $807.
The explanation from the pharmacy? “You haven’t met your deductible yet.”
That sounded plausible. It was January, the start of a new plan year. But when I logged into my portal, I saw something even stranger.
I had paid over $1,000 for medications in January, but my “Deductible Met” counter was sitting at $0.
Where did the money go? The system had bypassed the deductible entirely and applied the cash directly to my “Max Out-of-Pocket” limit.
- The Error: They were charging me full price (as if I had a deductible), but refusing to credit my deductible bucket.
- The Result: I was on track to pay thousands of dollars out-of-pocket without ever technically “meeting” my deductible. It was a phantom charge that left me with the worst of both worlds: high costs and no progress toward my coverage limits.
The Domino Effect: Why You Can’t Just “Let It Slide”
You might be tempted to just pay the overcharge to avoid the hassle. I understand that urge completely. But here is the trap: Insurance systems use something called an “accumulator.” It tracks how much you’ve paid toward your deductible.
If you pay a deductible that you don’t actually owe, the system “learns” the wrong information. Later, when you see a doctor or go to the hospital, their claims might get stuck or rejected because the math doesn’t add up. By fixing this one pharmacy error, I wasn’t just saving money on a prescription—I was unblocking thousands of dollars in medical claims that were stalled in the system.

Red Flags: How to Spot an Error
Unfortunately, we had already paid for the medications. Although the error was corrected in the “Carefirst” and Caremark.com com systems as of February 2, 2026 (excepting my order receipts), we did not receive a refund or even notification that a refund was due.
In fact, after speaking with several representatives this week it seems the “correction” was backdated; however, neither Caremark nor the local pharmacy where we bough a medication were told we were owed refunds. Our local pharmacy credited us the money for their end, now I am trying to get a refund from Caremark.
Here is how to know if you should question a charge:
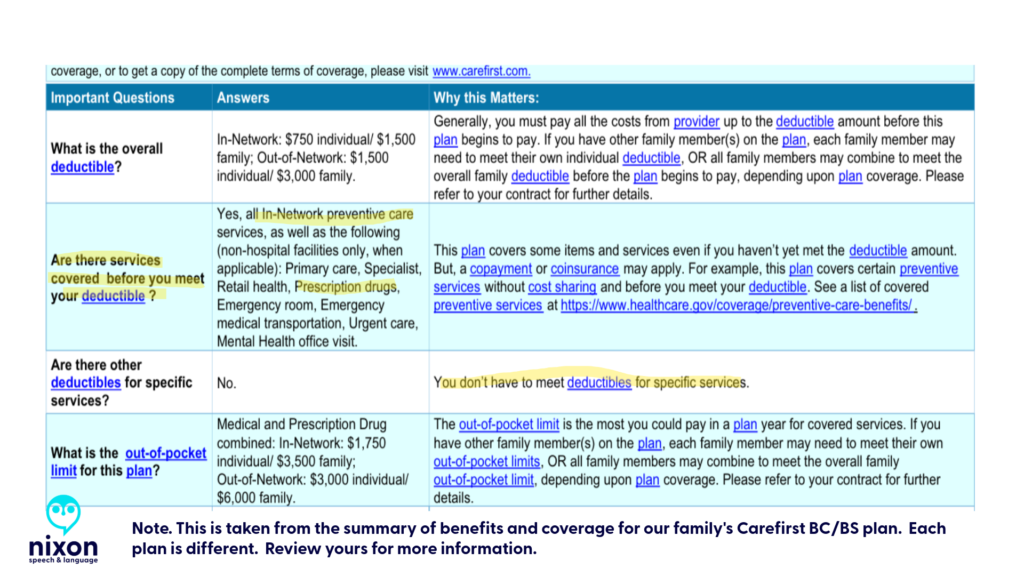
- The “Deductible” Surprise: If you have a PPO or HMO, your prescriptions usually have flat copays (e.g., $15, $30, $60) that apply immediately. If you see the word “Deductible” on a pharmacy receipt, check your plan design.
- The “Phantom Payment”: Check your insurance portal after a big purchase. If you paid $500 at the pharmacy, your “Deductible Remaining” should drop by $500. If the money disappears into the ether (or only hits your “Out-of-Pocket Max”), the system is miscoded.
- The “Processing” Limbo: If your medical claims (doctor visits) are sitting in “Processing” for weeks, it often means the medical system is waiting for the pharmacy system to send data that—thanks to this glitch—will never arrive.

Strategy: Write First, Call Second
The Reality: Phone calls are exhausting. But sometimes, secure messages result in frustrating, boilerplate responses that don’t answer your question. (I received a generic reply about “brand name drugs” that had nothing to do with my actual billing error!)
My advice: Even if you know you’ll have to call, send a Secure Message first.
- It creates a legal timestamp. Even if their reply is useless, you have proof that you reported the error on “Date X.” They can no longer say, “We have no record of that issue.”
- It forces a written response. When you finally do get a human on the phone, you can cut the small talk: “Please open Case #12345. I have already submitted the details in writing.”
- It respects your energy. If you have to file a formal legal grievance later, showing that they ignored your clear written explanation makes your case much stronger.
Pro-Tip: Document Like a Clinician
When you are dealing with brain fog or fatigue, relying on memory is risky. I treat every insurance interaction like a patient case note.
- Log Everything: Date, Time, and the Representative’s Name.
- Ask for the Reference Number: Every call has a “Case ID.” Ask for it immediately.
- The “30-Day” Clock: If they say they will “review it,” mark your calendar for exactly 30 days later. If they haven’t fixed it, they may owe you interest.
- See my post on creating a “patient’s log” that may help you track who said/did what (and when)
The Magic Words to Use
If you do have to speak to someone, use these terms to get past the front-line script:
- “Plan Design Error”: This tells them the computer is set up wrong for your specific group.
- “Adjudication Breakdown”: This asks for the math behind the price (e.g., how much was copay vs. deductible).
- “Accumulator Adjustment”: This asks them to fix your deductible history so future claims process correctly.
- “Senior team”: If you have already worked with the senior team on your issue, then explain the time it has taken and ask for the appropriate representative
The Takeaway
It took weeks of persistence, but we finally got a break. A representative worked with our local pharmacy on one claim and we were refunded for the discrepancy that was initially erroneously classified “deductible” ($747 of the $807.07 prescription cost). The call was disconnected before he could let me know how he was managing the issue with the Caremark pharmacy payments, but we have the proof we need to win.
I spent years advocating for others. Now, I’m learning that the most important advocacy is often the kind we do for ourselves—quietly, methodically, and with the receipts to prove it.
Disclaimer: I am a Speech-Language Pathologist and educational consultant, not an insurance broker or attorney. This post shares my personal experience and is not intended as legal or financial advice. Always consult your specific plan documents for coverage details.
Access and advocacy chronic illness claims processing clinical documentation bias communication log deductible Department of Education doge Dyslexia education errors processing claims gmail google workspace Guava Health Health apps healthcare communication disparities health insurance health insurance appeals health insurance benefits health insurance mistakes Independent Funding innovation Institute of Education Sciences invisible illness Kanban Task Tracker learning disabilities managing your health max out of pocket medical gaslighting examples medical record transparency more than labs National Institutes of Health neurodivergence NIH Organizer patient advocacy in healthcare Perplexity Health AI petition pharmacy benefit managers Planner Research Funding speech-language pathology Spoonie life subjective vs. objective medical notes Systematic Research
deductible, errors processing claims, health insurance, health insurance mistakes, max out of pocket, pharmacy benefit managers
When Your Insurance Company Suggests Insurance Company Suggests Medical Impossibilities – Nixon Speech and Language
[…] This post is a direct follow-up to my previous guide on auditing your Explanation of Benefits (EOBs). […]